-
Board-Certified
Fellowship-Trained
Physical Medicine
& Rehabilitation
Injection Therapy
 Injection therapy is intended to be a means to an end. The goal is to provide the patient with enough pain relief to bridge from inactivity to physical therapy, where back problems can be better treated with special exercises. For years, spine physicians have used cortisone injections, epidural steroid injections, trigger point injections and nerve blocks to relieve pain in the spine.
Injection therapy is intended to be a means to an end. The goal is to provide the patient with enough pain relief to bridge from inactivity to physical therapy, where back problems can be better treated with special exercises. For years, spine physicians have used cortisone injections, epidural steroid injections, trigger point injections and nerve blocks to relieve pain in the spine.
Epidural Injections
Epidural injections of cortisone may reduce the inflammation and/or swelling of the nerves in the epidural space resulting in decreased pain, tingling and numbness. The procedure involves inserting a needle of a long lasting steroid (cortisone) through the skin and deeper tissues into the epidural space. The epidural space is the area surrounding the spinal cord and the nerves coming out of it. One or more injections may be needed to relieve symptoms.
Facet Injection
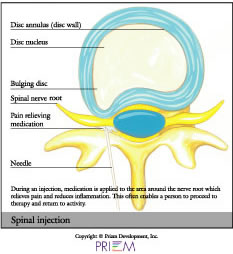
The facet joints act as the hinges in our back, connecting alll the vertebral bones in our back yet still allowing us to bend and twist with ease. The illustration above shows a facet injection in progress.
Sometimes from injury or age, these joints can become irritated or they can develop bone spurs, which makes movement painful. To relieve pain symptoms and restore range of motion, the spine physician may inject medication into the facet joint. The medicine in a way can act like WD40 on a rusty door hinge, restoring movement. Typically injections are done as a way to bridge the patient to therapy so the therapist can help the patient retain mobility after the effects of the medication wear off.
Trigger Point Injections
Trigger points are painful tissues in and around muscles. Pressure can cause an aching or sharp pain sensation. Trigger point injections are the administration of a local anesthetic and steroid medication in the muscles where pain is occurring. The injection may relieve spasms of the muscle and may last from weeks to months.
Sacro-Iliac (SI) Joint Injections
A long lasting steroid (cortisone) is injected into the sacro-iliac joint to help decrease inflammation and/or swelling of tissue in the joint space. As a result, patients may experience reduced pain and other symptoms caused by inflammation of the joint. The sacro-iliac joint is located in the low back area. The procedure involves inserting a needle through the skin and deeper tissues into the SI joint. More than one injection may be needed for symptom relief.
Rhizotomy
Rhizotomy is where the physician may use heat or cold to intentionally damage the ability of a problematic nerve to telegraph pain signals to the brain.
Radiofrequency Ablation
Radiofrequency ablation is a procedure used to reduce pain using a high-frequency radio wave to heat up a small area of nerve tissue, thereby decreasing pain signals from that specific area. Radiofrequency ablation is performed on an outpatient basis and requires only local anesthetic and mild sedation, and involves applying heat to certain nerve pathways to "shut off" the transmission of pain signals to the brain. This minimally invasive procedure can provide lasting relief to those suffering from facet joint pain or for patients that experience chronic back and neck pain from the degeneration of joints.
The procedure has a high success and low complication rate and can provide pain relief for up to 2 years. More than 70% of patients treated with Radiofrequency Ablation experience pain relief and is generally well-tolerated, with very few associated complications. Radiofrequency ablation is a proven safe way to help reduce pain with little to no side effects.
The only notable side effect of Radiofrequency Ablation is discomfort, which may include swelling and bruising at the site of the treatment, but this generally goes away after a few days.
COOLIEF
COOLIEF Cooled Radiofrequency is a minimally invasive outpatient treatment option that targets nerves that are causing chronic pain.
This advanced procedure uses cooled radiofrequency energy to safely target the sensory nerves causing pain. The COOLIEF system circulates water through the device while heating nervous tissue to create a treatment area that is larger than conventional RF treatments. This combination targets the pain-causing nerves without excessive heating, leading to pain relief. Some of the benefits of this procedure may include providing chronic back pain patients with up to 24 months of pain relief, improved physical function, and reduced prescription drug intake. It is common for the patient to feel some pain and discomfort at the site of the procedure for about a week, which can be reduced with ice packs and over the counter pain relief mediation.
Physician Biographies
-
 Karl Boellert, MD
Karl Boellert, MD -
 Mathew Gowans, MD
Mathew Gowans, MD- Board-Certified
Physical Medicine
& Rehabilitation
- Board-Certified
-
 Michael P.B. Kilburn, MD
Michael P.B. Kilburn, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
-
 Sumeer Lal, MD
Sumeer Lal, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
-
 John Cole, MD
John Cole, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
Back to Life Journal

Home Remedy Book

![]() Website Design & Educational Content © Copyright 2023 Prizm Development, Inc.
Developing Centers of Excellence for Better Healthcare.
Website Design & Educational Content © Copyright 2023 Prizm Development, Inc.
Developing Centers of Excellence for Better Healthcare.
Prizm is the most experienced developer of spine and orthopedic centers in the U.S. with content-rich educational web sites for physicians.
