-
Board-Certified
Fellowship-Trained
Physical Medicine
& Rehabilitation
Surgery
 If nonsurgical treatment options have failed, or if there are
If nonsurgical treatment options have failed, or if there are
emergency symptoms, spine surgery may be necessary.The spine surgeons at South Carolina Spine Center each perform a high volume of spine surgery each year—typically well over 200 cases annually. They are also fellowship-trained (the highest level of training possible) and board-certified. They concentrate their practice exclusively on spine surgery. Their expertise includes minimally invasive spine surgery, all common surgical problems in the neck and low back, scoliosis surgery, as well as new innovations including total disc replacement. In addition, the surgeons at South Carolina Spine Center are already referred some of the most complex spine cases across the region and have extensive experience with cervical myelopathy, scoliosis and deformity surgery as well as revision surgery. This experience translates into improved patient care of all spinal problems.
Leaders in spine surgery technology
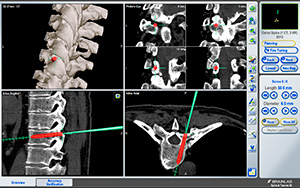
Image ©Brainlab, Inc., Used with Permission
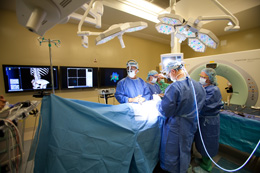
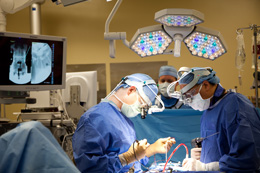
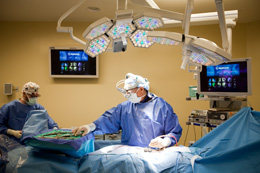
Surgeons at Self Regional Healthcare’s South Carolina Spine Center in Greenwood, SC are now treating patients with a variety of spinal conditions in its new advanced surgical operating room (OR) featuring Brainsuite® iCT from Brainlab.
Using the Brainsuite® iCT technology, complex revision procedures can now provide pain relief to patients who have undergone spine surgery elsewhere and had less than optimal results.
Image above shows the Brainsuite navigation screen when a pedicle screw is being placed in the spine.
Self Regional continues its commitment to advanced spinal care by becoming the first institution in the Southeast to use this highly advanced OR technology.
Integrating navigation with diagnostic quality intra-operative images offers tremendous benefit to the patient. The surgeons can perform with a higher level of accuracy in terms of instrument placement, supported by the ability to check that a surgical outcome has been achieved prior to concluding the procedure. This advanced technology has taken the OR to the next level.
Brainsuite iCT is a digitally integrated OR that combines image-guided surgery (IGS), with a multi-slice intra-operative computed tomography scanner (iCT) and comprehensive OR data management. The CT travels on rails over the OR table, providing high-quality intra-operative scanning without waking the patient from anesthesia.
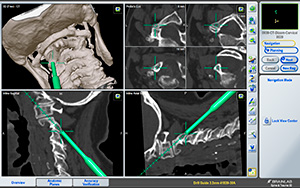
Image ©Brainlab, Inc., Used with Permission
It drives access to real-time imaging and enriched patient data that surgeons can use to make timely and informed decisions, as well as obtain pre-closure verification of results. Brainsuite iCT can be used for neuro, spine, ENT, cranio-maxillo-facial, trauma and orthopedic surgeries.
Image to the left shows the Brainsuite navigation screen of the cervical spine.
With the digital data management system Brainsuite® Net, patient data from the hospital’s Picture Archiving and Communications System (PACS) is accessible in the OR. Automatic Image Registration from Brainlab supports instant patient registration of intra-operative images without the need for fiducial markers or landmark recognition for seamless and time-saving navigation for surgeons. The VectorVision® sky navigation platform displays patient data collected during surgery and is equipped with two infrared cameras that verify the patient’s position in the OR.
This surgical navigation system integrates 3-D images from a CT scanner in the operating room with realtime guidance of instrumentation that functions much like a GPS system, but is incredibly more accurate. South Carolina Spine Center neurosurgeons can see images of the spine, discs and nerves during surgery and confirm placement within 1 millimeter. It provides the highest level of precision and accuracy available anywhere in the world, but its located right here in South Carolina.
The following is a list of common surgical problems and issues.
Cervical Spine / Neck
 Discectomy is the removal of the herniated portion of a disc to relieve the pressure on nearby nerves as they exit the spinal canal. Contrary
to myths, the disc does not slip out of position like a watermelon
seed. Instead, the disc is like a jelly donut, acting as the functional
shock absorber between two bony vertebrae. An injury, damage from a
lifting incident or a twist may cause the jelly center to break through
the wall of the disc. When a disc herniates, the jelly center can press
on nearby nerves. In the neck, this causes arm, shoulder, scapula and,
in extreme cases, spinal cord compression.
Discectomy is the removal of the herniated portion of a disc to relieve the pressure on nearby nerves as they exit the spinal canal. Contrary
to myths, the disc does not slip out of position like a watermelon
seed. Instead, the disc is like a jelly donut, acting as the functional
shock absorber between two bony vertebrae. An injury, damage from a
lifting incident or a twist may cause the jelly center to break through
the wall of the disc. When a disc herniates, the jelly center can press
on nearby nerves. In the neck, this causes arm, shoulder, scapula and,
in extreme cases, spinal cord compression.
Posterior Cervical Foraminotomy / Discectomy
For some herniated discs or bone spurs in the neck affecting only the nerve roots, a posterior discectomy and foraminotomy can be performed. This avoids spinal fusion, and with a microscope or a minimally invasive technique, can minimize recovery time and speed a patient back to work or activities.
Anterior Cervical Discectomy
Cervical is the medical term for "neck." Just as in a lumbar discectomy, the surgeon will remove a piece of damaged disc tissue in the neck area to relieve pressure on the spinal cord or nerve roots. In some cases, by removing a piece of the shock-absorbing disc that separates the two vertebrae, the structures may become less stable. Consequently, when the disc is removed, a surgeon may recommend "fusing" the vertebrae to prevent instability. A cervical discectomy is best left to surgeons who specialize in spine.
Corpectomy
 A corpectomy is often performed for patients suffering from multiple
levels of cervical stenosis with cord compression. The goal of a
corpectomy is complete decompression of the spinal canal when stenosis
encompasses more than just disc space and has moved into vertebral
bodies.
A corpectomy is often performed for patients suffering from multiple
levels of cervical stenosis with cord compression. The goal of a
corpectomy is complete decompression of the spinal canal when stenosis
encompasses more than just disc space and has moved into vertebral
bodies.
Bone spurs forming toward the back of a vertebral body or the ligament behind vertebral bodies can cause the cervical spinal canal to narrow. Therefore, it may be necessary to remove one or more degenerating vertebrae and the discs above and below in order to decompress the spinal cord and nerve roots.
A corpectomy involves a vertical incision in the neck. The middle portion of the vertebra and its adjacent discs are removed to achieve decompression of the cervical spinal cord and nerve roots. A fusion accompanies a corpectomy surgery, using bone harvested from the patient's hip or from a bone bank. This bone graft is used to reconstruct the spine and provide stability.
Anterior Cervical Fusion
A fusion accompanies a anterior cervical discectomy or corpectomy. During fusion surgery, a disc Is removed, and the surgeon inserts a small wedge of bone between two vertebrae to restore disc space. Over time, the two vertebrae "fuse" together into a single solid structure. While this procedure limits movement and flexibility, it also helps relieve neck pain.
Bone graft for the purpose of spinal fusion may be harvested from the patient's hip (autograft bone), from a cadaver bone (allograft bone), or from synthetic bone graft substitutes, which are currently being developed more extensively. Your surgeon will help you decide what is best for you.
Laminoplasty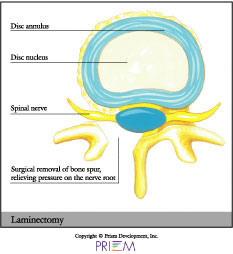
A laminoplasty, similar to a laminectomy, is often performed on patients
suffering from spinal stenosis in the neck (narrowing of the cervical
spinal canal). It is also referred to as an "open-door laminoplasty." A
laminoplasty creates more space for the spinal cord and roots. The
actual procedure involves cutting a “hinge” into one
side of the lamina and swinging it open like a door. It relieves
pressure on the spinal cord by increasing the diameter of the spinal
canal and room for the spinal cord. The surgery approach is through
the back of the neck. This procedure creates excellent spinal canal
decompression without the instability that may be created by multiple
level cervical laminectomies.
[top]
Lumbar surgery/low back
Microdiscectomy / Minimally invasive discectomy
Discectomy is the removal of the herniated portion of a disc to relieve the pressure on nearby nerves as they exit the spinal canal. Contrary to myths, the disc does not slip out of position like a watermelon seed. Instead, the disc is like a jelly donut, acting as the functional shock absorber between two bony vertebrae. An injury, damage from a lifting incident, or a twist may cause the jelly center to break through the wall of the disc. When a disc herniates, the jelly center can press on nearby nerves. This causes back or leg pain when the hernation is in the low back, and arm pain if the disc is in the neck area (see "cervical spine/neck").
 In a lumbar discectomy, the surgeon typically only removes
the portion of the disc that is causing a problem, not the entire disc.
If you have a herniated disc, keep in mind that a disc has a purpose.
When you remove a disc, it may cause instability in the joint, and
a surgeon may recommend a fusion to re-stabilize the area.
In a lumbar discectomy, the surgeon typically only removes
the portion of the disc that is causing a problem, not the entire disc.
If you have a herniated disc, keep in mind that a disc has a purpose.
When you remove a disc, it may cause instability in the joint, and
a surgeon may recommend a fusion to re-stabilize the area.
The surgeon can remove the damaged piece of disc through a traditional incision in the back. However, at South Carolina Spine Center, the surgeons typically use a microscope to minimize incision size, tissue trauma and recovery time. In addition, in some cases, minimally invasive discectomy can provide an even less invasive approach.
Depending on the nature of your disc problem, your surgeon will recommend the most appropriate type of surgery for you.
Posterior lumbar interbody fusion (PLIF)
 This spinal fusion surgery is very similar to the anterior lumbar interbody
fusion, except that the surgeon approaches the spine through the low
back. This method is used when there is a greater amount of instability
in the patient's spine. An advantage to this surgery is that it can
also provide anterior fusion of the disc space without having a second
incision.
This spinal fusion surgery is very similar to the anterior lumbar interbody
fusion, except that the surgeon approaches the spine through the low
back. This method is used when there is a greater amount of instability
in the patient's spine. An advantage to this surgery is that it can
also provide anterior fusion of the disc space without having a second
incision.
Lumbar laminectomy
A laminectomy involves the removal of part or all of the bone covering the spinal canal. The purpose of this procedure can be to free nerve roots, remove a tumor, bone spur or to perform certain types of fusion procedures. Removing the lamina (laminectomy) is much like removing the cover on a fuse box to access the wiring. By removing the lamina, the surgeon gains access to the disc area and frees more space for the nerves inside.
A laminectomy in the lumbar spine is often used to treat
recurrent disc herniations or where scar tissue is involved. Laminectomy
may also be used in cases of spinal stenosis in which the entire canal
is narrowed like a ring on a swollen finger, squeezing all of the nerve
roots at that level of the spinal canal.
[top]
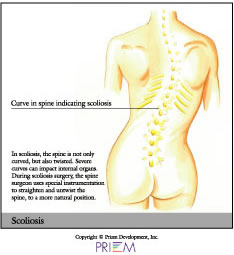 Scoliosis & spinal deformity
surgery
Scoliosis & spinal deformity
surgery
Through the placement of hooks, rods and screws, a spinal curve can be corrected and stabilized. A fusion often follows scoliosis surgery, in order to maintain the correction permanently.
Scoliosis is not the result of an injury and usually appears without cause. It can be inherited, and it usually affects more women than men. In the case of most spinal curves, the spine is not only bent but also twisted like a bent corkscrew. Some cases of scoliosis are not serious. Over time, if a curve worsens, surgery may be required to correct the curve and prevent pain and worsening deformity. In extreme cases, if the curve is not corrected, the spinal deformity can place pressure on internal organs, which can shorten a person's life expectancy.
During scoliosis surgery, the surgeon may use special
instruments that attach onto various vertebra segments. These surgical
rods are the adjusted to "de-rotate" the twisted and bent
corkscrew spine. Decades ago, Harrington Rods (the “first-generation” of
instrumentation) were used to surgically straighten the spine. However,
this technique did not untwist or correct the spine. Today, there are “fourth-generation” techniques
to improve corrections, minimize levels fused and minimize the need
for post-operative bracing.
[top]
Spinal fusion
Unusual movement at a vertebral segment will probably result in pain, especially if the person already has or displays symptoms of degenerative disc disease, fractures, scoliosis or a weak spine. This movement may require a discectomy, and subsequently, a lumbar interbody fusion. Anterior and posterior fusion techniques can be performed in the neck and the low back.
 Not all patients who have spinal problems need spine
surgery. They can be managed with microscopic decompression or minimally
invasive techniques. Spinal fusion is reserved for patients who have
spinal instability, spinal deformity or painful degenerative pain.
Obviously, this is only after a patient has failed all conservative
measures.
Not all patients who have spinal problems need spine
surgery. They can be managed with microscopic decompression or minimally
invasive techniques. Spinal fusion is reserved for patients who have
spinal instability, spinal deformity or painful degenerative pain.
Obviously, this is only after a patient has failed all conservative
measures.
In fusion surgery, the goal is to cause bone graft to
grow between two vertebrae and stop the motion at a particular segment
by adding bone graft to it. This results in one long bone rather than
two separate vertebrae. Anterior and posterior lumbar fusions may be
done separately or can be used together for the most severe problems
of the cervical (neck), thoracic (chest level) and lumbar spine (low
back). Your spinal surgeon will help you decide which technique is
right for you.
[top]
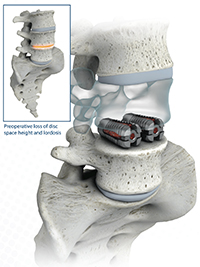
Image copyright © Wenzel Spine Inc.
Varilift
The Vari-Lift® is the only stand-alone solution for spine stabilization that eliminates the need for rods and screws to treat multiple spine disorders like disc herniation, degenerative disc disease, adjacent level disease and spondylolisthesis. The tool offers a minimally invasive approach to a fusion surgery.
In a traditional spinal fusion, a four-inch incision is made to access the vertebrae, followed by the insertion of bone grafts or other materials to fuse the bones. Other instrumentation is put in place to keep the spine stable while the fusion heals.
By contrast, using a smaller incision, the small VariLift-L® device is installed between the vertebrae, resulting in faster recovery time and less pain during recovery.
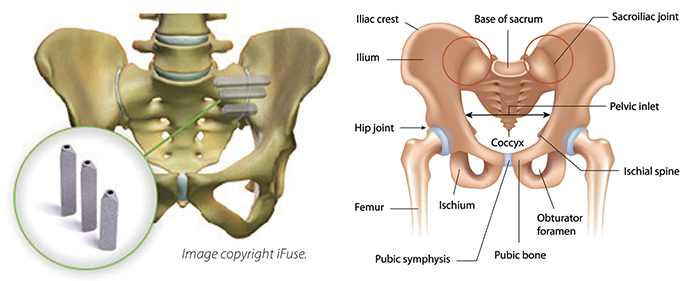
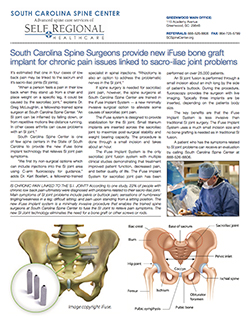
i-Fuse Bone Graft for SI Joint pain
IS CHRONIC PAIN LINKED TO THE S.I. JOINT? According to one study, 22% of people with chronic low back pain ultimately were diagnosed with problems related to their sacro-iliac joint. Main symptoms of SI joint problems include pelvis or buttock pain; sensations of numbness/ tingling/weakness in a leg; difficult sitting; and pain upon standing from a sitting position. The new iFuse implant system is a minimally invasive procedure that enables the trained spine surgeons at South Carolina Spine Center to fuse the SI Joint to relieve pain symptoms. The new SI Joint technology eliminates the need for a bone graft or other screws or rods.
“When a person feels a pain in their low back when they stand up from a chair and place weight on a specific leg, it could be caused by the sacroiliac joint,” explains Dr. Michael Kilburn, a fellowship-trained spine surgeon at South Carolina Spine Center. “An SI joint can be inflamed by falling down, or from repetitive motions like distance running. In other cases arthritis can cause problems with an SI joint.”
South Carolina Spine Center is one of few spine centers in the State of South Carolina to provide the new iFuse bone implant technology that relieves SI joint pain symptoms.
Click here to download
If spine surgery is needed for sacroiliac joint pain, however, the spine surgeons at South Carolina Spine Center are trained in the iFuse Implant System — a new minimally invasive surgical option to alleviate some causes of sacroiliac joint pain.
The iFuse system is designed to provide stabilization for the SI joint. Small titanium implants are inserted across the sacroiliac joint to maximize post-surgical stability and weight bearing capacity. The procedure is done through a small incision and takes about an hour.
The iFuse Implant System is the only sacroiliac joint fusion system with multiple clinical studies demonstrating that treatment improved patient function, decreased pain, and better quality of life. The iFuse Implant System for sacroiliac joint pain has been performed on over 25,000 patients.
An SI joint fusion is performed through a small incision about an inch long by the side of patient’s buttock. During the procedure, fluoroscopy provides the surgeon with live imaging. Typically three implants are be inserted, depending on the patients body size.The key benefits are that the iFuse Implant System is less invasive than traditional SI joint surgery. The iFuse Implant System uses a much small incision size and no bone grafting is needed as in traditional SI fusion.
A patient who has the symptoms related to SI joint problems can receive an evaluation by calling South Carolina Spine Center at 888-526-8806.

Image copyright © Medtronic.
Artificial disc
At South Carolina Spine Center, Dr. Michael Kilburn uses the Bryan® cervical disc for certain patients with herniated discs in the neck who would otherwise need a spinal fusion. With traditional spinal fusion, two vertebrae are “fused” together with a bone graft. While this common surgery retains the disc height after a damaged disc is removed, the fusion locks the two vertebrae together which can in turn put increased stress on the disc levels above and below as the neck rotates. That can cause additional disc herniations above and below the fusion site. This is called "adjacent segment disease."
The benefit of an artificial disc is that it retains the normal motion of the disc which reduces the risk of adjacent segment disease.
For more information about artificial disc technology, click here.
Physician Biographies
-
 Karl Boellert, MD
Karl Boellert, MD -
 Mathew Gowans, MD
Mathew Gowans, MD- Board-Certified
Physical Medicine
& Rehabilitation
- Board-Certified
-
 Michael P.B. Kilburn, MD
Michael P.B. Kilburn, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
-
 Sumeer Lal, MD
Sumeer Lal, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
-
 John Cole, MD
John Cole, MD-
Board-Certified
Fellowship-Trained
Spinal Neurosurgeon
-
Board-Certified
Back to Life Journal

Home Remedy Book

![]() Website Design & Educational Content © Copyright 2023 Prizm Development, Inc.
Developing Centers of Excellence for Better Healthcare.
Website Design & Educational Content © Copyright 2023 Prizm Development, Inc.
Developing Centers of Excellence for Better Healthcare.
Prizm is the most experienced developer of spine and orthopedic centers in the U.S. with content-rich educational web sites for physicians.
